Jul 27, 2021
What began as an innovative tool that analyzed what Windsorites flush down the toilet, in order to more rapidly detect the prevalence of COVID-19 in the community, has since expanded to include testing at the other end of the digestive tract.

Dr. Qiudi Geng, a research associate at the University of Windsor test local waste water for traces
of the COVID-19 virus at the school on Monday, July 26, 2021. PHOTO BY DAN JANISSE /Windsor Star
Analyzing samples from both municipal sewage systems and human saliva in mouths, a multi-disciplinary team of scientists at the University of Windsor is aiming to now track and publicize diseases in the population before the negative health symptoms even begin to show.
And the public gets to see the ongoing results in an online real-time interactive dashboard that combines the results of this early sampling with disease outbreaks detected and reported by health authorities like the Windsor-Essex County Health Unit.
The monitoring so far has shown that what lurks in the mouth and what is expelled from the other end of the digestive tract can provide an earlier warning of disease in the community than having to wait for sick people to begin filling up hospital emergency rooms.

Ryland Corchis-Scott, a PhD student at the University of Windsor test local waste water for traces
of the COVID-19 virus at the school on Monday, July 26, 2021. PHOTO BY DAN JANISSE /Windsor Star
“We’re setting this up so it can be a surveillance (system) for any virus, pathogen or even food-borne illness,” said Lisa Porter, a biologist and executive director of the WE-SPARK health initiative. “We can monitor and be ahead of the game — instead of waiting for disaster.”
Assistant professor Pooya Moradian Zadeh and computer science masters students Farzaneh Jouyandeh and Sarvnaz Sadeghi created an online dashboard that provides real-time information on active and new COVID-19 cases in the community.
“The dashboard, combined with the wastewater and saliva screening, provides a surveillance platform to support the safe re-opening of Windsor-Essex,” said Porter.
“We’re supplementing the wastewater results we’re getting in Windsor and Essex County. It’s another piece of data to assess the situation,” said Mike McKay, executive director of the university’s Great Lakes Institute of Environmental Research (GLIER).
Local wastewater samples are collected three days a week at the city’s two sewage treatment plants and from facilities in Amherstburg, Lakeshore and Leamington. Results, some as soon as the next day, are posted on the dashboard and help health authorities get an earlier heads-up on any developing trend in COVID-19 community outbreaks.
“The public health community sees this as an early-alert — we shed the virus from our bodies before we see the symptoms,” said McKay, an expert in environmental microbiology. GLIER is doing the same effort in Chatham-Kent and in Thunder Bay, while most Ontario health units are now benefitting from similar monitoring.
McKay said the wastewater sampling can’t pinpoint exactly where an outbreak is occurring, but it does provide an early alert. “You can’t target a single area, but what you can do is launch public awareness campaigns — it’s a good reminder.”
Specific cases and outbreaks can be pinpointed, however, with the saliva testing, which Porter said the University of Windsor is hoping to take advantage of by the fall when the campus community begins to return in a limited capacity.
“This is a platform we can use as the community begins opening up,” said Porter.
There’s also hope the new tools and dashboard can be used in the future in order to avoid another massive disruption as was seen — and is still being felt — by COVID-19. The same monitoring, she and McKay said, can be used as an early warning system during the regular flu season or to detect community outbreaks of other viruses or pathogens or even food-borne illnesses.
While others in the community could take advantage of the same monitoring system now in place, Porter said the saliva testing is currently focused on the university community, with students volunteering to be tested. Subjects remain anonymous to those doing the research and monitoring, but, should their test come back positive, they will get an alert on their smartphones.
Sports teams are another possible application, said Porter, so that infected individuals can be isolated at an earlier stage. The samples are also being sequenced to determine what variants are present in the community.
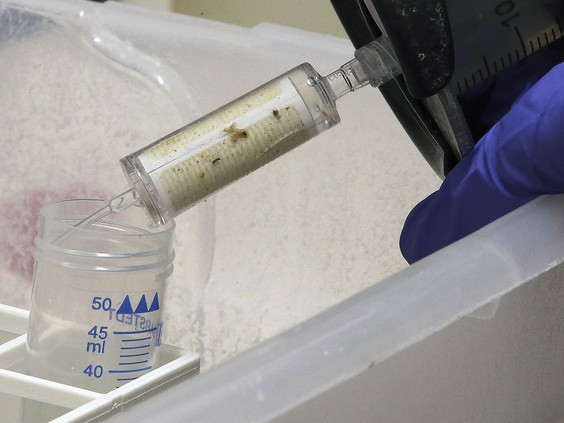
Ryland Corchis-Scott, a PhD student at the University of Windsor test local waste water for traces
of the COVID-19 virus at the school on Monday, July 26, 2021. PHOTO BY DAN JANISSE /Windsor Star
“One of the things we learned over the past year is that the wastewater (results were) mirrored in the clinical cases,” said Porter. That is, when the sewage testing coronavirus numbers rose, the number of reported actual coronavirus clinical cases in the community were found to subsequently rise as well.
“All of us want to get back to campus — this is one way we get there,” said Porter, adding: “It’s novel, its innovative … (and) as an early indicator, this is pretty cost-effective.”
Courtesy: https://windsorstar.com/news/local-news/uwindsor-early-detection-tools-warn-community-of-infectious-disease






